 These tests are used to answer a specific clinical question (eg, why is the patient short of breath?), and the results of each should be considered as either supporting or negating the pre-test probability of a suspected diagnosis. 
While spirometry and D LCO each have a lengthy list of indications related to specific disease entities, the clinical indications for measurement of lung volumes are less well defined.Īll the component tests of a complete PFT are measures of lung physiology. Spirometry provides the vital capacity (VC) or FVC and its components, inspiratory capacity (IC) and expiratory reserve volume (ERV), but must be combined with other methods (plethysmography, gas dilution, or imaging) to estimate the trapped volume. None of these volumes can be measured directly by spirometry each depends on measurement of the gas trapped in the lung after a maximal exhalation-the RV. Lung volumes in this context include measurements of total lung capacity (TLC) and its components, functional residual capacity (FRC) and residual volume (RV). In addition to spirometry, measurements of diffusing capacity of the lung for carbon monoxide (D LCO) and lung volumes have become de rigueur components of a “complete” pulmonary function test (PFT). The use of computer controlled pulmonary function equipment allows laboratories to perform an array of tests to investigate lung function in a repeatable and standardized manner. Newer approaches such as computed tomography, although not suitable for routine testing, may help to delineate the true underlying physiology. However, the differences between techniques are not completely understood. Body plethysmography is often considered more accurate than gas dilution methods in the presence of obstruction. How lung volumes are measured may be important, especially in patients who have moderate or severe airway obstruction. Changes in inspiratory capacity, RV, or FRC may be important gauges of response to bronchodilators or other hyperinflation-reducing therapies. The variability of lung volumes related to degree of obstruction suggests that measuring gas-trapping may be needed to monitor therapy. Hyperinflation and air-trapping are terms commonly used to reflect these changes, but are not well standardized. TLC may be normal, but is frequently increased in the late stages of COPD. Increased lung volumes, particularly residual volume (RV), are commonly observed in airway obstruction. In obesity, VC and TLC may remain within normal limits, but functional residual capacity (FRC) can exponentially decrease. Mixed obstruction-restriction and the nonspecific pattern (ie, reduced FVC and FEV 1, normal FEV 1/FVC and TLC) require measuring TLC to confirm the underlying physiology. This makes “physiologic” sense because, in healthy subjects, and in patients with true restriction, VC comprises most of the total lung capacity (TLC). A restrictive pattern can have many etiologies, and clinicians often use VC or FVC as a primary index of lung volume. Confirming “restriction” when vital capacity (VC) or FVC is reduced is perhaps the most important. 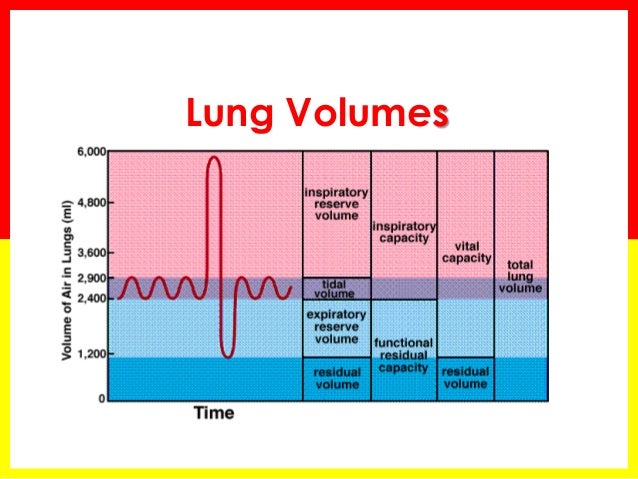
Unlike spirometry and diffusing capacity of the lung for carbon monoxide (D LCO), which do contribute to confirming or excluding a diagnosis, there are few clear indications when lung volumes are discriminatory. Lung volumes are considered part of a complete pulmonary function test, but their value for enhancing clinical decision making is unknown. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
